2020-10-15 / News
A guest article by Schwindt E., Jung P., Jessie M, Heimberg, Hoffmann, Deindl P., Härting H., Schwindt J.
Since the outbreak and the worldwide spread of SARS-COV-2 at the beginning of 2020, the entire world has changed. Over 1 million deaths worldwide are attributed to SARS-COV-2 in 2020 (data from October 1st). Lockdowns and restrictions revealed an impact on everyone, in one way or another. The medical world also changed, and a lot of us had to face challenges never seen before.
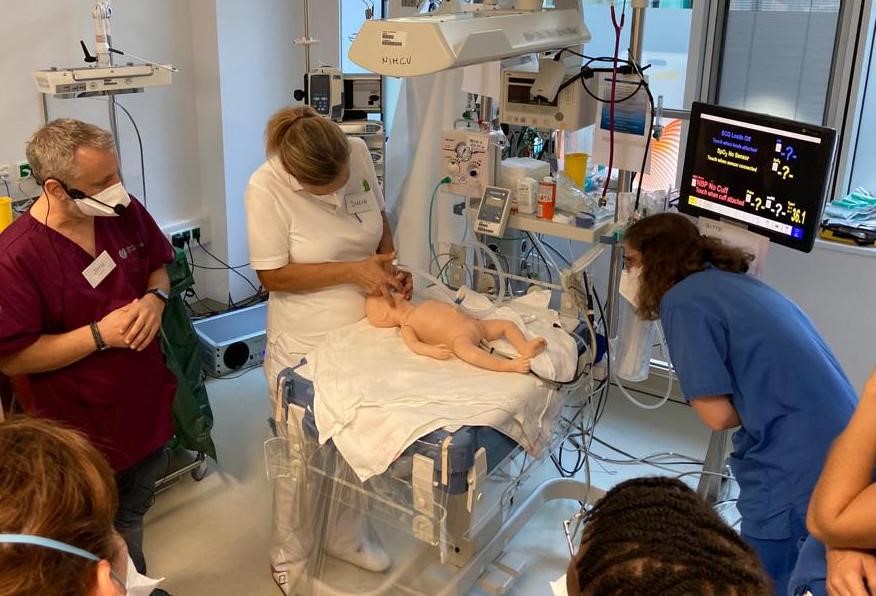
Familiarization during a high-end neonatal simulation training; trainers and participants wearing FFP-2 masks. ©SIMCharacters
Challenging times for continuous training
Unfortunately, due to understandable insecurities in managing the fragile balance between levity and overprotection during such difficult pandemic times, medical teams lost the possibility of training rare and complex situations because numerous medical training sessions have been cancelled. The fear of infection during training sessions and the temporary loss of critical, high-specialized medical team members often led to preventative handling of these situations. The medical world still seems to regard training as “a nice to have” or an “add on, if there is time”. In contrast to other high-risk areas, medicine still seems to suggest that medical teams’ training is an extravagance, every institution can decide on its own to provide it or not. Regarding this attitude, it is clear that in challenging times during a pandemic, training events are among the first activities to be cancelled.
However, we are humans and our skills will decrease rapidly if not repeated (45% performance decrease after only three months)[1]. If we do not train regularly, we will not be prepared to manage rare, complex, and dangerous situations, and we will not be able to keep patient safety on a high level. Training of technical skills (mechanical ventilation, resuscitation, intubation, etc.) and non-technical skills (leadership, teamwork, effective communication, etc.) are crucial to treat neonatal patients and to foster neonatal teams’ optimal performance.
Multiple studies show clear evidence that medical training improves individual performance[2–5], teamwork[6–11], safety culture and system safety[12–14], and patient outcome[15–17]. There is no doubt that we have to fight SARS-COV-2 infections with all our resources. Nevertheless, according to a recent WHO statistic, 2.628.000 patients die EVERY YEAR due to medical errors, only in low and middle-income countries[18]. These numbers make medical errors the third most common cause of death in the U.S., after heart disease and cancer. More people die due to medical errors than from all respiratory diseases and strokes together[19]. If we are not recognizing this as a global health priority and not treating this similar to a global pandemic, we are failing to live up to our responsibilities that we have in the health care system.
The significance of medical errors
Medical errors are challenging to measure and not a highly visible dimension compared to media-effective emergencies or human victims of a pandemic. If an Airbus 320 crashes, more than 200 people might die, and emotional pictures of grieving family members and airplane debris in the fields instantly demand immediate actions of responsible people, organizations, and legislative institutions to make sure that this will never happen again. In contrast, when an extremely preterm born infant of 500 grams birth weight dies, the baby’s death might be explained by claiming that it was just too immature, too small, or too sick to survive.
Still, we cannot objectively measure and compare medical performance, patient safety, and outcomes with other institutions to identify issues that require improvement. There still is not enough pressure to succeed in patient safety issues, although every minute, five patients die worldwide due to medical errors. The visibility of medical errors is low, and we still feel safe sending our family members into hospitals.
We strongly believe that medical teams must regularly train and exercise complicated procedures and situations, even during difficult epidemic times. We have to be aware that theoretical lessons or well-intentioned training videos alone will never reach the same effect as hands-on practical team training does. The haptic experience, the emotional aspects, and the team interaction during simulation training cannot be achieved by online training. As long as we have to work hands-on on patients and in teams, we also have to practice hands-on and in teams to provide optimal performance for our patients in real life.
Providing safe training
Based on our hands-on practical training experiences during the SARS-COV-2 epidemic, table 1 summarizes our suggestions to make training sessions as safe as possible. Further, details and careful considerations about training in pandemic times are available from the European Resuscitation Council and the Austrian Resuscitation Council[20,21].
It is a matter of course that we are in this together fighting against SARS-COV-2, but not at the expense of patient safety. Training is necessary, especially during a pandemic, highlighting how important well educated and trained medical staff is to save lives. In the light of the resources mobilized worldwide to fight against a common enemy like SARS-COV-2, there is no excuse not to mobilize all possible resources to fight against the silent killer medical error.
Therefore, medical teams’ practical hands-on training is one proven tool to enhance patient safety, and this is crucial before, during, and after a pandemic. During the pandemic, we need to ensure that training is still achievable safely for medical teams. After the pandemic, we must have an agenda involving political leaders, health ministers, health organizations, economists and healthcare providers and focus all our efforts to make regular team training available and mandatory for all medical professionals worldwide.
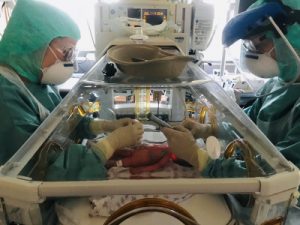
Simulated intubation training in a preterm born infant with COVID-19 infection in full personal protective equipment. ©SIMCharacters
| Issue | Explanation |
| Distant learning | Theoretical knowledge or introductions for practical training sessions might be provided using distant learning methods like video recordings or webinars during high-risk epidemic times with increasing numbers of SARS-COV-2 infections. According to the local situation, careful considerations have to be done to enable personal attendance for theoretical lessons. |
| Teaching videos | Teaching videos and other digitalized computer-based training can provide an optimal multiplication tool for theoretical knowledge or practical instructions – followed by hands-on training where indicated. |
| Low-threshold, regular skills training | Instead of long-time previously planned extensive training sessions, it is sometimes easier to train the team in a low-threshold manner, such as performing basic CPR training on a low-fidelity manikin during calm shifts. (frequent low-threshold, simple skills training). Ideally, this form of spontaneous training requires several trainers dedicated to this idea to serve as multiplicators. Nonetheless, if appropriate equipment is at hand (e.g. manikin), even the youngest team members can take the initiative to initiate low-fidelity training. |
| Masks | Trainers and trainees wear mouth nose masks (FFP 1 or FFP 2 according to pandemic activity) at all times during the training session. |
| Group size | We recommend a maximum group size of eight trainees, which must be adapted according to the available room size and the possibility to open windows. |
| Environment | Search for optimal rooms that enable to hold a distance of at least 1 meter (except during hands-on training, when e.g. working side-by-side on a patient), the possibility to open windows and vent sufficiently, separate chairs to a distance of at least 1 meter (respectively according to your local guidelines). |
| Obligation to regular training and request by management | Management has to demand their employees to complete defined training sessions on defined intervals to ensure that training sessions would be caught up later if indeed had to be cancelled. |
| Clinical briefing & debriefing | A considerable benefit can be taken out of real events if standardized briefing and debriefing are established. Beneath regular training sessions, we have to take maximal use out of real events. |
| Catch up after the pandemic | During the pandemic, the cancellations of training sessions lead to a loss of knowledge and practical skills of medical teams, which requires even more intensive training curricula after the pandemic. This already is custom in other high-risk areas like aviation, where licenses for pilots generally are restricted to six months (then training is obligatory) and after the SARS-COV-2 lockdown, an even more intensive re-entry training is required. |
With thanks to the authors:
Schwindt E1, Jung P2, Jessie M3, Heimberg4, Hoffmann5, Deindl P6, Härting H7, Schwindt J8
1Medical University Vienna
Department of Pediatrics and Adolescent Medicine
Division for Neonatology, Pediatric Intensive Care and Neuropediatrics
Währingergürtel 18-20
1090 Vienna, Austria
2University Hospital Schleswig-Holstein
Department of Pediatrics and Adolescent Medicine
Campus Lübeck
Ratzeburger Allee 160
23538 Lübeck, Germany
3Bürgerhospital Frankfurt am Main – Clementine Children’s Hospital
Department of Neonatology and Pediatric Intensive Care,
Nibelungenallee 37-41
60318 Frankfurt am Main, Germany
4University Children’s Hospital Tübingen
Department of Pediatrics
Hoppe-Seyler-Straße 1
72076 Tübingen, Germany
5Dr. von Hauner Children’s Hospital
Ludwig-Maximilians-University
Department of Emergency Medicine and Pediatric Critical Care Medicine
Lindwurmstr. 4
80337 Munich, Germany
6University Medical Centre Hamburg-Eppendorf
Children’s Hospital
Department of Neonatology and Pediatric Intensive Care Medicine
Martinistr. 52
20246 Hamburg, Germany
7Assekurisk Safety Management GmbH
Wiegelestraße 2
1230 Vienna, Austria
8Austrian Resuscitation Council
Pediatric Working Group
Villefortgasse 22
8010 Graz, Austria
References
1 Anderson R, Sebaldt A, Lin Y, Cheng A. Optimal training frequency for acquisition and retention of high-quality CPR skills: A randomized trial. Resuscitation. 2019;135:153–61.
2 Dugan MC, McCracken CE, Hebbar KB. Does Simulation Improve Recognition and Management of Pediatric Septic Shock, and If One Simulation Is Good, Is More Simulation Better? Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc. 2016;17(7):605–14.
3 Halamek LP, Kaegi DM, Gaba DM, Sowb YA, Smith BC, Smith BE, et al. Time for a new paradigm in pediatric medical education: teaching neonatal resuscitation in a simulated delivery room environment. Pediatrics. 2000 Oct;106(4):E45.
4 Hunt EA, Duval-Arnould JM, Nelson-McMillan KL, Bradshaw JH, Diener-West M, Perretta JS, et al. Pediatric resident resuscitation skills improve after “rapid cycle deliberate practice” training. Resuscitation. 2014 Jul;85(7):945–51.
5 Minai F, Shafiq F, Ul Haq MI. Value of real life (in situ) simulation training for tracheal intubation skills in medical undergraduates during short duration anesthesia rotation. J Anaesthesiol Clin Pharmacol. 2014 Oct;30(4):484–7.
6 Auerbach M, Roney L, Aysseh A, Gawel M, Koziel J, Barre K, et al. In situ pediatric trauma simulation: assessing the impact and feasibility of an interdisciplinary pediatric in situ trauma care quality improvement simulation program. Pediatr Emerg Care. 2014 Dec;30(12):884–91.
7 Kurosawa H, Ikeyama T, Achuff P, Perkel M, Watson C, Monachino A, et al. A Randomized, Controlled Trial of In Situ Pediatric Advanced Life Support Recertification (“Pediatric Advanced Life Support Reconstructed”) Compared With Standard Pediatric Advanced Life Support Recertification for ICU Frontline Providers*: Crit Care Med. 2014 Mar;42(3):610–8.
8 Mileder LP, Urlesberger B, Szyld EG, Roehr CC, Schmölzer GM. Simulation-based neonatal and infant resuscitation teaching: a systematic review of randomized controlled trials. Klin Padiatr. 2014 Sep;226(5):259–67.
9 Rubio-Gurung S, Putet G, Touzet S, Gauthier-Moulinier H, Jordan I, Beissel A, et al. In situ simulation training for neonatal resuscitation: an RCT. Pediatrics. 2014 Sep;134(3):e790-797.
10 Thomas EJ, Williams AL, Reichman EF, Lasky RE, Crandell S, Taggart WR. Team training in the neonatal resuscitation program for interns: teamwork and quality of resuscitations. Pediatrics. 2010 Mar;125(3):539–46.
11 Schmutz JB, Meier LL, Manser T. How effective is teamwork really? The relationship between teamwork and performance in healthcare teams: a systematic review and meta-analysis. BMJ Open. 2019 Sep;9(9):e028280.
12 Kurup V, Matei V, Ray J. Role of in-situ simulation for training in healthcare: opportunities and challenges. Curr Opin Anaesthesiol. 2017 Dec;30(6):755–60.
13 Riley W, Begun JW, Meredith L, Miller KK, Connolly K, Price R, et al. Integrated Approach to Reduce Perinatal Adverse Events: Standardized Processes, Interdisciplinary Teamwork Training, and Performance Feedback. Health Serv Res. 2016 Dec;51:2431–52.
14 Riley W, Meredith LW, Price R, Miller KK, Begun JW, McCullough M, et al. Decreasing Malpractice Claims by Reducing Preventable Perinatal Harm. Health Serv Res. 2016 Dec;51 Suppl 3:2453–71.
15 Mduma E, Ersdal H, Svensen E, Kidanto H, Auestad B, Perlman J. Frequent brief on-site simulation training and reduction in 24-h neonatal mortality–an educational intervention study. Resuscitation. 2015 Aug;93:1–7.
16 Okuda Y, Bryson EO, DeMaria S, Jacobson L, Quinones J, Shen B, et al. The Utility of Simulation in Medical Education: What Is the Evidence?: UTILITY OF SIMULATION IN MEDICAL EDUCATION. Mt Sinai J Med J Transl Pers Med. 2009 Aug;76(4):330–43.
17 Riley W, Davis S, Miller K, Hansen H, Sainfort F, Sweet R. Didactic and simulation nontechnical skills team training to improve perinatal patient outcomes in a community hospital. Jt Comm J Qual Patient Saf. 2011 Aug;37(8):357–64.
18 Committee on Improving the Quality of Health Care Globally, Board on Global Health, Board on Health Care Services, Health and Medicine Division, National Academies of Sciences, Engineering, and Medicine. Crossing the Global Quality Chasm: Improving Health Care Worldwide. Washington, D.C.: National Academies Press; 2018.
19 James JT. A new, evidence-based estimate of patient harms associated with hospital care. J Patient Saf. 2013 Sep;9(3):122–8.
20 ERC. European Resuscitation Council [Internet]. Pathw Resuming ERC Courses Peak Level COVID-19 Pandemic. 2020 Oct [cited 2020 Oct 5]. Available from: https://erc.edu/sites/5714e77d5e615861f00f7d18/pages/5e9ac62b4c84867335e4d1eb/files/20200602_ERC_COVID19_-_Section_9_-_Pathway_4.pdf?1592906300
21 ARC. Austrian Resuscitation Council [Internet]. Durchführ Von Kursen Zur Aus- Fortbild Während COVID-19-Pandemie. 2020 Oct [cited 2020 Oct 5]. Available from: https://www.arc.or.at/covid/
You are currently viewing a placeholder content from Facebook. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More InformationYou are currently viewing a placeholder content from Instagram. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More InformationYou are currently viewing a placeholder content from X. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More Information